
Mapping Care Together
Sept - Nov 2025
Individual Project · Master Level · Industrial Design Engineering
Course: Capita Selecta
This project explores how patient journey mapping can be redesigned to better include older adults in healthcare design. Healthcare systems are often complex and fragmented, making it challenging for patients to navigate their experiences, particularly in later life. While patient journey mapping is widely used to understand care experiences, existing approaches often overlook individual perspectives and may not be accessible or intuitive for older participants. This independent individual project was conducted as part of the Ageing Right Care(fully) (ARC) project, a transnational research initiative focused on ageing in the home environment and the development of hospital-at-home care.
Problem Statement
Healthcare journeys are often mapped, but rarely told by the people who experience them. Although patient journey mapping is widely used to understand care experiences, it is typically shaped by researchers rather than patients themselves, which can limit how accurately lived experiences are represented. This is especially relevant for older adults, who may face barriers when engaging with traditional methods due to differences in communication, accessibility, and cognitive load. Literature highlights the importance of empowerment, co-design, and inclusion, emphasising that patients should play an active role not only in sharing but also in interpreting their experiences. This calls for a shift from extracting information to enabling participation, where methods are adapted to support diverse needs and create more meaningful engagement. This project therefore asks:
How can patient journey mapping workshops be effectively adapted to meet the unique needs of older adults?
Design Principles
Based on insights from the literature and early exploration, a set of design principles was developed, focusing on clarity, accessibility, and participation. These principles were used to guide the design of the workshop and mapping tools, ensuring that the process would be inclusive, easy to engage with, and supportive of active participation by older adults.
1. Use plain and simple language and explain unfamiliar or technical terms clearly.
2. Provide information and materials in multiple formats, such as visual, textual and verbal, to support comprehension and engagement.
3. Offer translation or communication in participants’ preferred language where possible.
4. Create an atmosphere of empathy, safety and mutual respect that encourages honest sharing and emotional comfort.
5. Be transparent about who is involved, the purpose of the mapping and how the process and results will be used.
6. Clearly communicate participants’ roles and describe the methods, tools and visuals in accessible and understandable terms.
7. Involve participants in reviewing and interpreting findings to ensure authenticity and shared understanding.
8. Encourage active participation and co-creation by inviting participants to share their stories, reflections and lived experiences.
9. Respect participants’ time and energy by keeping sessions well-structured, purposeful and flexible.
10. Avoid overburdening participants by allowing breaks, adjusting pacing and adapting activities to individual comfort levels.
Concept
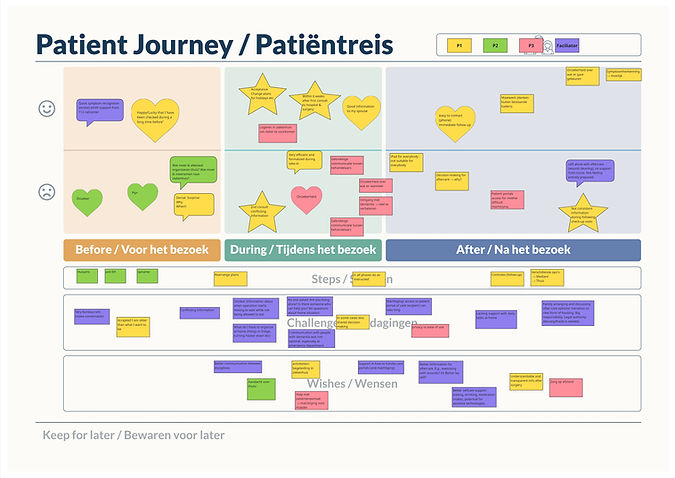
The concept is a co-design workshop built around a shared patient journey map that participants fill in together. The journey is structured into three phases: before, during, and after care, with the “after” phase given more space, reflecting the focus on hospital-at-home experiences. The map includes sections for challenges, wishes, and “keep for later” to capture not only what happened, but also opportunities for improvement and points that fall outside the main flow.
The workshop is designed for multiple participants working collaboratively on the same map. A dedicated space is included for participants to write their names, ensuring that contributions can be recognised and traced back if needed. Each participant is assigned a specific colour of sticky notes, which helps distinguish individual inputs while still maintaining a shared and collective overview. To further structure the input without making it complex, different sticky note shapes are used to represent types of information, for example, feelings, thoughts, and general notes. This visual coding system makes it easier to quickly understand the content on the map, supports memory during the session, and helps guide participants in how to contribute without requiring detailed instructions.

Workshop & Findings
The concept was tested through a small, in-person co-design workshop with older adult participants. The session was set up around a large, shared journey map placed at the centre of the table, creating an open and collaborative setting. Participants worked together using coloured sticky notes and markers, moving through the three phases of the journey step by step. The atmosphere was informal and conversational, which encouraged participants to share their experiences freely and build on each other’s input.
During the session, it became clear that the process worked best as a discussion rather than a structured task. Many of the most valuable insights emerged through conversation, with participants helping each other recall details and reflect on their experiences. At the same time, the workshop revealed some challenges. The use of multiple sticky note shapes and visual elements sometimes caused confusion, increasing cognitive load and making it harder for participants to keep track of what each element represented
After the workshop, the journey map was digitised to preserve the content, organise the information more clearly, and make it easier to share with participants and other stakeholders. This step also allowed for reflection and validation, ensuring that the captured experiences remained accessible beyond the physical session. A key insight from the results was the importance of experiences outside the hospital itself. Participants consistently reflected on moments before and especially after care, highlighting challenges in recovery, communication, and follow-up. These phases were often described as more impactful than the hospital experience alone, reinforcing the decision to place greater emphasis on the “after” stage.
Recommendation
Future development will focus on refining the method to make it clearer, more intuitive, and easier to engage with. Simplifying the visual elements and reducing complexity will help lower cognitive load and improve accessibility for a wider range of participants. The approach will be tested with a larger and more diverse group to better understand its applicability across different contexts. Combining group workshops with follow-up or individual sessions will provide deeper, more personal insights. In the longer term, the method will be explored within real healthcare settings, for example, as part of patient feedback or service evaluation, while the digitised journey maps will support communication between patients, caregivers, and healthcare professionals.
Reflection
Through this project, I learned a lot about co-design in practice and developed a strong interest in healthcare design. Working directly with participants showed me how valuable these methods are, but also how challenging they can be, especially when working with multiple people at once. I experienced first-hand how group dynamics and language differences can affect the flow of a session, and how important it is to stay flexible as a facilitator. Overall, it helped me better understand what it means to design with people rather than for them.





